Your Knee Pain Diagnosis Begins Here
You’ve got two of them. As far as you know, both are the same age. So why is it that it seems so often that one knee bothers you more than the other? And why the heck are we so darn prone to knee pain?
In this article, I’m going to cover:
- Some basic knee anatomy
- Why most common medical treatments are such a bad idea
- Surgery seems inevitable with time…but is it?
- Supplements for arthritis
- Treatments you HAVE to have done for knee pain
- Long term strategies for knee health
So grab a cup of coffee or glass of wine (depending upon the time of day) and get comfortable.
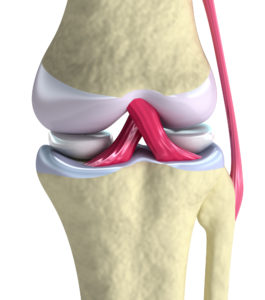
Some Basic Knee Anatomy
You’ve been looking down at them your entire life (or just staring at them in the mirror if you haven’t seen over your belly in a decade) but have you really considered how they are put together?
The knee is basically a hinge joint. Much like the elbow, the main movement for the knee is flexion and extension, although some degree of rotation does occur. The technical name for this is a ginglymus joint and in anatomy terms it’s referred to as genu (for those of you church-goers, if you ever wondered why the heck it was called “genuflect” as you bent your right knee as a sign of reverence, now you know).
Bones and Ligaments Involved in a Knee Pain Diagnosis
It is made up of the meeting of 3 bones, the femur (thigh bone), tibia (shin bone) and fibula. The top and bottom of these bones form a very smooth surface at the ends, creating the knee joint. The knee joint is held in place by a few ligaments that are designed to keep the knee from moving too far in a direct it’s not designed to go. These ligaments are:
- The lateral collateral ligament (LCL—on the outside)
- The medial collateral ligament (MCL—on the inside)
- The anterior cruciate ligament (ACL—keeps the tibia from sliding forward too far)
- The posterior cruciate ligament (PCL—does the opposite—keeps the femur from sliding forward off the tibia)
The surface of the bones contains the cartilage, which has mainly two different types—the hyaline cartilage covering the bones and the menisci, which acts as a shock absorber for the joint. You’ve probably heard that there are two menisci; one on the outside (lateral) and one on the inside (medial) and that the medial one is pretty darn prone to injury (more on this later).
Muscles Involved in a Knee Pain Diagnosis
The muscles that surround the knee are basically made up of the front and back sets of muscles. The muscles in the front straighten your knee (called extension). There are four of them (hence the reference to your “quads”): quadriceps femoris, rectus femoris, vastus lateralis, vastus medialis.
The muscles that flex your knee are the semimembranosus, semitendinosus and biceps femoris (collectively referred to as your hamstrings). While the gastrocnemius muscle can flex the knee, it is not usually considered as a knee flexor.
There are a few other muscles that are important in knee movements. You’ve most likely heard of the iliotibial band (aka ITB), but the actual muscle is the tensor fascia latae (TFL). The ITB is the fibrous band of tissue that is affected by the muscle, but is not actually muscle tissue.
While the TFL is mainly involved in hip motion, it can play a large role in what causes knee pain because it attaches to the tibia and is prone to irritation (more on this later as well). Since it attaches to the outside portion of the knee, it can play a role in rotating the knee outwards.
The Sartorius muscle is the longest muscle in the human body and wraps from the front of the pelvis to the inside of the knee. It is also referred to as the “Tailor’s muscle,” which stems from the position that a tailor would sit in to sew. It helps to flex the knee and rotate it inward. It meets up with three other muscles to form the pes anerine. Bursitis in this area is possible.
The gracilis is also a muscle that attaches to the inside of the knee at the pes anserine as well. It is much more involved in hip movements, but it does help with flexing the knee.
Bursa as a Cause of Knee Pain
Bursae are little lubricating sacs that the body puts in areas around joints that would otherwise generate a lot of friction. This is all fine and dandy until something goes wrong and then, instead of creating pain-free movement, all movements involving the bursa are painful.
While there is a long list of bursae surrounding the knee, there are a few that create more frequent problems:
- Pes anserine bursitis—as already mentioned, this is the bursae on the inside of the knee underneath the sartorius, semitendonosis and gracilis. Can be a common cause of pain on the inside of the knee.
- Suprapatellar bursa—underneath the quadriceps just as it inserts into your kneecap.
- Infrapatellar bursa—just below the kneecap. Inflammation in the area in a growing child can also be a sign that Osgood-Schlatter Disease may be starting (luckily, this can usually respond really well to treatments we will cover later in this article).
- The bursa that can cause pain behind the knee is referred to as a Baker’s cyst when it becomes enlarged enough to cause pain behind the knee.
Probably the most important thing I can say here is that a “bursitis” is almost always the consequence and not the cause. In other words, your knee burse do not suddenly burst into inflammation for no good reason.
There is always a cause for the bursitis. Settling for a diagnosis of “bursitis” and being happy with being giving a steroid injection is the absolute wrong attitude if you truly hope to keep your knees functioning for decades to come.
Fascia as a Cause of Knee Pain
Ahhhh. How to I begin this portion of the article?? The portion that discusses the tissue that is so incredibly overlooked and undertreated?
I’ve always had a hard time communicating to patients just what the fascia is because it’s so darn complicated and unique. There is nothing I can point to in a car, a manufacturing plant or even on TV.
The closest I have come is a piece of chewing gum. It’s warm, it’s pliable, it’s moist, you can hold things together with it and stretch it in all kind of directions. Simplistic, but it seems to work. (in case you’re looking for a deeper understanding, you can check out Thomas Myer’s Anatomy Trains videos on YouTube)
So. You’ve got this gum holding everything together. And then, you add a piece of ice to the mix and the gum hardens up and loses all of the characteristics I just mentioned.
Putting all other tissues that I have mentioned aside and focusing only on the fascia of your knee, it surrounds EVERYTHING. It connects EVERYTHING. It is a critical component of how EVERYTHING moves around the knee joint.
I know that I just covered the ligaments of the knee a minute ago. However, current theories are actually debunking the idea that ligaments truly exist.
Rather, they are thickenings of the fascia along areas of a joint that provide increased stability. We have called them ligaments and have seen them on cadavers because anatomists have dissected out what they were looking for. In other words, they were looking for a ligament so, as they dissected out a region they actually created the ligament from the fascia surrounding that area. So, this thickening of tissue exists, but it is actually the continuation of the fascia from the area above and below it.
So what does this mean?
It means that the fascia surrounding a joint may be the most critical tissue that needs to be addressed for joint pain.
Mess with the fascia and the dynamics and balance of your knee goes out the window. But we’ll go over this later in the article and how to treat the causes of knee pain.
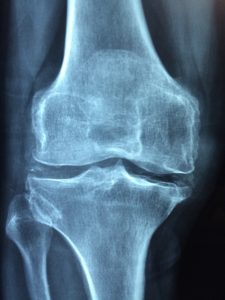
Pain Inside the Knee; What About X-rays and MRIs?
Before we get past the anatomy of the knee and onto more meaty stuff, there is one topic that needs to be addressed before everything else.
Imaging of the knee.
Whether we’re talking about plain X-rays, an ultrasound (not typically done on the knee, but it can be used), MRI or CT scans, they all add information to the clinical picture of what is going on with pain inside the knee.
But is more information better?
I think the answer to that question is a very solid NO. MRIs for back pain lead to more epidurals and surgery. PSA testing for prostate cancer leads to unnecessary surgeries. Mammography has not been shown to lower the rate of breast cancer deaths, but it does create a massive spike in surgery and chemotherapy.
But the knee is much more straightforward when it comes to information from imaging studies. Besides, doesn’t everyone want an MRI. It’s cool to take a peek inside your body without the downsides of autopsy. But for pain inside the knee does an MRI help anything?
I firmly believe, based on the research and my own clinical experience, that most knee pain does not come from arthritis, but rather from pain being created in the soft tissues (muscles, ligaments, tendons, fascia) surrounding the knee joint as well as the imbalance and altered stress placed upon the joint by these damaged soft tissues.
To back this up, consider what happened when a group of researchers looked at patients who were older than 50 without any signs of knee osteoarthritis on X-rays to see if MRI images added any additional information. On MRI, the researchers looked for abnormalities that are associated with knee osteoarthritis:
- osteophytes (also known as bone spurs)
- cartilage damage
- bone marrow lesions
- subchondral cysts
- meniscal lesions (usually described as a torn meniscus)
- synovitis
- attrition (a wearing down of the joint surface)
- ligament lesions
What they were basically doing was looking at MRI as a tool to see how well findings on an MRI compared with what the patient was experiencing. Here’s what they found:
- 89% of the group had at least one abnormality noted above (osteophytes were the most commonly found at 74%, followed by cartilage damage in 69% and bone marrow lesions in 52%.
- As expected, the prevalence of abnormalities went up with age.
- The likelihood of at least one type of abnormality was high in both painful (97%) and painless (88%) joints.
The last point being the most important. Basically, over the age of 50, a MRI becomes less and less important, and may lead the unsuspecting physician to recommend a more invasive procedure (injection or worse–knee replacement).
The bottom line is that just because you have something wrong on your MRI, particularly as you get older, does not guarantee that it means anything.
It might, but until you try approaches that I’m going to cover in this article, you’d be making a mistake if you jumped on something as drastic as a knee replacement first.
If the approaches outlined in this article do not help, you can still opt for more invasive procedures. But the reverse doesn’t work so well…
The Dangers of Drugs and Surgery for Arthritis Knee Pain Relief
There is a definite path to medical treatment for the causes of knee pain.
This path starts with rest and some anti-inflammatories like ibuprofen or something maybe a little stronger.
If this doesn’t work, you’ll get an X-ray. When nothing shows up broken then maybe you’ll get another 2 weeks of so of anti-inflammatories for your arthritis knee pain relief.
When the knee pain is STILL there, a MRI is next on the list of things to do.
From there, a course of therapy to strengthen your already strong knee is next (weakness of a muscle rarely causes knee pain by itself). If you’re lucky you’ll get some electric stim and ultrasound. Maybe even laser if the clinic is hip on new technology.
The end path for this course is some type of surgery. Just arthroscopic or, if your surgeon happens to be in a very gracious mood, full-blown knee replacement.
Seems pretty typical.
But may not in your best interests. But which part should you avoid?
Maybe like all of it…?
What about Medications for Arthritis Knee Pain Relief?
Western medicine uses medication as its principle tool. If you’ve read any of my articles, like..ever, you know that all too often the downside of medications do not balance out the upside.
Since it is so darn common to use medications to manage knee problems, this section is designed to enlighten you to the dangers of using these medications. That way, if you still choose to use them you do so understanding the risks fully.
Opioid Pain Relievers for Arthritis Knee Pain Relief
If you’ve just emerged from a cave (AND managed to get a computer and Internet access) in the past few weeks, I would not be surprised if you weren’t aware that the Opioid Crisis has pretty much been considered a national emergency.
While the US Government was spending our money and efforts on stopping illicit drug use, in the background medicine was slowly building a society that not only condoned prescription narcotic drug use, but PAID FOR IT!
Then, beginning at least in 2008, the number of deaths associated with prescription narcotic use exceeded those deaths caused by illicit drug use. It still took a few years after this, but this was essentially the waking up period for deaths from prescription narcotic use.
Codeine, OxyContin, Percocet, Vicodin, morphine, Xanax and Valium (these last 2 are benzodiazapines–but frequently abused), Valium, Tramadol, Tylenol 3.
It never ceases to amaze me how quickly prescriptions for narcotic pain relievers are given out. In the ER it is almost a given. High likelihood in urgent care. Still far too common in a primary care settings.
But it’s just a simple prescription, right?
All too often it’s a slippery slope to continued use.
One study looked at just this problem. While this article looked at analgesic use after low risk surgery (gall bladder, cataract, TURP for prostate enlargement and varicose vein stripping) and not specifically at knee pain, it’s not about the procedure but rather about the use of pain relievers and the mindset that goes with their use. The results were surprising:
- Within 7 days of discharge, a new prescription for opioids were given to 7.1% of patients.
- If an opioid prescription was given to a patient within 7 days of surgery, they were 44% more likely to become a long term user (still using after a year).
- NSAIDs were prescribed to 0.3% within 7 days of discharge but jumped to 7.8% at 1 year from surgery
- Those taking NSAIDs within 7 days of surgery were almost 400% more likely to become long-term NSAID users.
Wow. Talked about generating a society that is addicted to drugs. And while this study looks at low risk surgery, how similar would the numbers be for neck pain? Low back pain? Knee pain or headache? Makes me happy to be a chiropractor.
Again, I would ask…is the “War on Drugs” looking at the wrong side of the prescription pad?
Anti-Inflammatories for Arthritis Knee Pain Relief
If the body is so brilliantly designed, why does it seem to be so prone to chronic musculoskeletal complaints?
There are injuries and situations that result in more tissue damage and have a higher chance of leading to chronic pain. Think skiing, skateboarding or snowboarding injury. High speed car crashes. Motorcycle accidents. Equestrian wipeouts. Surgery.
But what about the weekend warrior who pulls a hamstring? The 8 hour per day computer user? Or me, as a lifelong martial artist, who has had untold injuries over the decades to pretty much every area of my body? Why do these situations lead to chronic pain?
My personal thought (backed by lots of research and years of clinical practice) is that the development of chronicity has much to do with how we handle the immediate period after the injury or onset of symptoms. What do the vast majority of us do (which is, of course, the direction indicated by billions of dollars of advertising) in this immediate period?
Rest. Ice. Pop an over the counter pain reliever or anti-inflammatory.
This is arguably the worst possible combination possible.
Why?
First, there’s the immobilization. Within minutes of immobilization, the soft tissues surrounding your joints begin to change for the worse. The longer a joint is kept from moving, the worse the tissue damage.
Anyone who’s ever broken a bone and had it casted can attest to how much joint motion is lost once the cast comes off. Recovery time is usually longer than the casting itself.
With any tissue injury, the size of the region that ends up being affected is larger than the original injury size. Consider the swelling associated with an ankle sprain—the area of the ligament injury may actually be very small, but the entire ankle, foot and lower leg swells up to the size of a balloon and becomes discolored within a short period of time.
Because of this, the amount of tissue that becomes injured is much larger than the original injury. As healing occurs, unless the injured tissue undergoes movement in the proper fashion, healing will happen haphazardly.
I’d like to compare this to a small leak in your bathroom faucet. You call in the plumber. He shows up with a crew that’s been drinking at the bar for half the day. They proceed to rip out half the bathroom to fix the leak and rebuild with a level of skill only a non-Irishman on St. Patrick’s Day can achieve.
Your body is no different.
As we heal after an injury, the new tissue, whether it is bone, muscle, ligaments, fascia or tendons, is laid down in a disorganized manner. Only as that region goes through movement do these healing tissues become stressed and rebuild along the lines of force.
For this reason, immobilization becomes the enemy of proper healing.
The second action that sets you up for chronic pain is the routine use of over the counter or prescription anti-inflammatories. All anti-inflammatory medications interfere with the inflammatory process.
Unfortunately, inflammation is a part of the normal process of healing. Block it and you disrupt the ability of your body to heal the way it was designed.
Compare anti-inflammatories to the use of ice right after an injury. Ice works simply by slowing blood flow to the newly injured area, keeping the damage done by the drunken plumbing crew from getting out of control in the first place.
With this in mind, you should begin to understand that the combination of immobilization and anti-inflammatory drugs may be the first step in developing chronic pain.
Repeat this cycle every time you get injured the problems just get worse.
One study looked at just how much non-steroidal anti-inflammatories (NSAIDs) effect healing after rotator cuff surgery tendon repair in a study in rats. Researchers found that every case was affected, from complete failure of healing to tissue that was much weaker.
While this study did not look at the knee specifically, the effect of NSAIDs on the healing process is still the same. Luckily, over time surgeons have recognized this bad interaction and tell their patients to avoid NSAIDs for 6-8 weeks after the surgery.
NSAIDs for Arthritis Knee Pain Relief; A Dangerous Combination
Just in case the fact that anti-inflammatories derail proper healing wasn’t enough to convince you, what if the very drugs you took to stop the pain in your knees was destroying them?
Sound a little far-fetched?
For at least the past THIRTY YEARS, we have known that NSAIDs block the metabolism of the cells that make up your joint surface-the chrondrocytes.
By taking anti-inflammatories long term, you are pretty much ensuring that you are going to destroy the very joints you’re trying to protect. And not just the knees—this damage will occur on every joint surface in your body.
Some anti-inflammatories are worse than others (diclofenac always seems to be at the top of the list of the bad guys), but they all contribute to the slow death of your joints.

What about Surgery for a Knee Pain Diagnosis?
So maybe drugs aren’t a good idea. Like ever (as it relates to knee pain).
But certainly, there’s a place for surgery, right?
Not nearly as often as you would think. And consider this-there is absolutely no doubt that any type of surgery done on the knee will speed up the development of arthritis in that knee, especially if a torn meniscus is removed.
Knee Replacements for Arthritis Knee Pain Relief
No one ever wakes up in the morning with a hankerin’ for major surgery involving the bones of your knee, Dewalt power tools and carpentry techniques.
Rather, many get to the point where they feel that surgery is the only option left, with a complete knee replacement being the most aggressive option for those whose knees are shot.
Knee pain is a pretty common complaint in my office. Many times, patients have been told that their knee pain is arthritis and there is basically nothing that can be done except for a knee replacement.
This is frequently not the case.
It is common for a patient to come into my office, only to leave 2 or 3 visits later with much less pain in their knees. Did the arthritis suddenly get fixed? Of course not. Rather, the pain was not coming from the joint itself, but rather from the fascia surrounding the knee.
But surely patients would never have their knees replaced because of something that could otherwise be fixed if he or she got to the right type of physician…
Right?
Look at what researchers found when they looked at why there was such a big spike in in the number of knee replacements being done in the US. They were thinking that there would be a parallel increase in the amount of arthritis being found on imaging, confident that this increase was due to the increased obesity and the increasing age of the population.
This was not what they found. Rather, knee pain increased without any relationship to age and BMI.
Of extreme importance is what they did NOT find.
They did NOT find an increase in arthritis of the knee.
Western medicine is performing more and more knee replacements, but it’s not due to obesity or age. Nor are we performing more knee replacements because of more arthritis found on imaging.
Basically, we are replacing potentially good knee joints because of problems due to fascia surrounding the joint that was never effectively treated.
I will again assert that anyone with knee pain should first be evaluated by a physician that specializes in the treatment of the soft tissues that surround the knee. If pain persists after several visits, then an evaluation by a surgeon may be warranted, but certainly not before.
Arthroscopic Knee Surgery for Arthritis Knee Pain Relief
I’ve already covered the fact that there is very little connection between imaging findings and what causes knee pain.
In other words, if someone has “stuff” wrong on a MRI, it does NOT mean this person is going to have pain. You cannot look at a MRI and state that this patient will or will not have pain.
This fact leads to a really big problem.
The orthopedic surgical field is entirely based on doing procedures based on stuff found on imaging. Got a disc bulge on MRI? Cut it out. Have knee osteoarthritis on X-ray? Replace the knee. Torn rotator cuff on MRI? Surgical repair of the shoulder.
A review of 9 research studies looked at the question of whether or not there was a benefit to doing arthroscopic surgery arthritis knee pain relief—basically a “clean out” of the knee. In these studies, middle aged and older patients with knee pain and degenerative knee disease (diagnosed with imaging studies) underwent knee arthroscopic surgery.
The notable thing about these studies were that they were some of the very first studies ever to use a placebo group for surgery. I’m sure you can understand that there is a stigma with cutting someone open just to cut them open for the benefits of a research study. The first of these placebo-knee-surgery were done in a military hospital setting in 2002 at the Houston VA medical center.
Here’s what the researchers found 2 years had passed after surgery:
- There was almost no benefit to surgery (the real one) in patients’ pain levels (basically, a benefit of 2.4 mm on a 0-100 mm scale).
- There was no benefit on physical function.
- While there was no benefit over placebo, the surgical group’s harms included symptomatic deep venous thrombosis, pulmonary embolism, infection, and death.
It’s pretty clear that going in for surgery just to “clean out” the knee has virtually no benefit but a list of risks. Thankfully, it seems like, while being very popular for many years (upwards of 800,000 of these types of surgeries per year in the US alone), this is a procedure that is not really done anymore.
Some of that may have more to do with insurance not paying than with surgeons paying attention to what the research advises.
Orthopedic surgeons, however, are still very commonly doing surgery for cartilage tears and knee ligament tears (like the ACL).
Pain Inside the Knee: Surgery for ACL tears
The anterior cruciate ligament, as I described above, checks the motion of the tibia on the femur (keeps it from sliding too far forward). It is a commonly injured ligament of knee, usually occurring when the body is rotated on a planted knee (think soccer and football injuries).
In general, once you tear your ACL you’re out of luck. If you’re still relatively active, the recommendation is typically to have surgery to use a tendon from your hamstring or a tendon from a cadaver to replace your torn ligament. If you’re past your active days, surgery is not as strongly recommended.
But what if this thought process, like so much else we have believed to be true, is not the entire story?
A medical study followed 121 young active adults with ACL tears raises questions about the dogma that exists on the need for surgery for many knee conditions. Basically, delaying surgery and trying non-surgical management first seems to be the better option.
Here’s the specifics:
- 62 of those with ACL tears were put in rehab and had early ACL reconstruction, with 59 assigned to rehab (surgery later only if still needed)
- Of the group who initially did not have surgery, 39% ultimately had ACL reconstruction.
- Based on the Knee Injury and Osteoarthritis Outcome Score (KOOS, which asks about pain, symptoms, function in sports and recreation, and knee-related quality of life), there was NO difference in any of the treatment approaches.
In other words, just because you have an ACL tear does NOT mean that you have to have surgery. It makes complete sense to go into rehab after an injury like this with the expectation that you will not need surgery, but keeping an open mind about the potential need for ACL reconstruction if you do not respond to rehab.
Pain Inside the Knee: Surgery for Degenerative Meniscus Tears
I’ve already pointed out that there is little evidence to support surgery for debridement or a “clean out” for arthritis knee pain relief. Even though this evidence began to emerge as early as 2002 (15 years ago as of the writing of this article), I really don’t think that many surgeons truly changed behaviors.
From an insurance standpoint, if the surgeon was looking to get a surgery approved for a “clean out,” it is just as easy to say he or she was going in to fix a meniscal tear. This sounded like a good idea because the back part of the medial meniscus (posterior horn) is commonly torn and does not have a very good blood supply to assist with nutrient delivery for healing. Thus the rationale for surgical intervention to go in and remove the torn meniscus.
There are a couple of problems with this thinking.
The first is one that I’ve already pointed out– MRI is not an exact science and that, if something is “found” on MRI, these findings may not be the causes of knee pain.
This is not to say that that torn medial meniscus on your MRI is not causing you pain, it’s just that we can’t know for sure. I can tell you, from treating hundreds of knees over the years, that a huge chunk of knee pain comes from the soft tissues surrounding the knees (muscles, ligaments, fascia) and not from what is going on inside the knee.
Fix these tissues and the knee pain goes away, regardless of whether or not the meniscus is affected by the treatment. (again—more on this later in the article).
The second problem has to do with a study looking to answer the question whether surgery to repair a degenerative meniscus tear (as opposed to one that happens from trauma) actually does squat.
Specifically, researchers were interested in whether self-reported locking or catching would be improved by partial meniscectomy.
Seventy patients underwent the real surgery to remove a portion of the medial meniscus and 76 had a fake surgery done. Here’s what they found:
- 46% in the true surgery group reported catching or locking before surgery; after surgery that number was 49% (yes—it actually went up).
- Of the fake surgery group, 49% reported catching or locking before surgery; after “surgery” the number was 43% (yes—the numbers went down).
In other words, some $50,000 later, risk of infection, down time for recovery and pain for rehab, there was pretty much no difference between the groups.
Studies like these and the other ones mentioned in this article are blowing open the doors of the dogma that surrounds knees injuries, findings on MRI and the value of arthroscopic surgery.
This is not to say that there is not value to the surgical options, but you better damn well be sure you see someone who truly understands how to assess and treat the soft tissues surrounding the knee before you go under the knife.
Pain Inside the Knee: Surgery for Traumatic Meniscus Tears
We’ve already seen that surgery just to “clean out” a knee isn’t any better than non-surgical treatments. Same with the majority of ACL tears. Ditto for degenerative (age-related) meniscal tears.
But certainly if you tear your meniscus playing soccer or weekend warrior flag football (or, for the less-than-should-be-active of you, stepping off a curb) it’s going to need surgery.
As I already mentioned, the meniscus does not have a very good blood supply. For this reason, we’ve always thought that the meniscus does not heal well from an injury and needs to be removed surgically.
I personally had my right knee scoped when I was 18 for a medial (inside) meniscal tear while playing football (would have loved to have blamed in on 4 years of gymnastics, but managed it while being tackled). Surgery seemed like a good idea at the time, and at the time I was never really aware of an alternative.
Just like the other scenarios I have outlined, for a long time there were no studies looking at outcomes of surgery for a traumatic meniscal tear versus not having surgery.
Until this study was published in the British Medical Journal comparing outcomes after a year between 397 patients who had surgery for degenerative meniscal tears versus surgery for traumatic meniscal tears.
Here’s the details:
- Outcomes from surgery used the knee injury and osteoarthritis outcome score (KOOS) that cover pain, symptoms, sport and recreational function, and quality of life.
- Patients with degenerative meniscal tears had more improvement in KOOS4scores than those with traumatic tears.
- Almost half of patients with traumatic tears were not satisfied with their current knee function one year after arthroscopic partial meniscectomy.
While this study doesn’t completely clarify things, it does give us some things to think about.
First, the outcomes for surgery on degenerative meniscal tears was slightly better than that for traumatic tears. Given that I’ve shown that surgery wasn’t more effective than non-surgical approaches for degenerative tears, this really doesn’t instill confidence in me for how well surgery works for traumatic tears.
Second, half of those who had surgery were not happy with the outcomes one year later. There is a distinct possibility that this is because, in addition to any damage to the meniscus, the soft tissues surrounding the knee were also damaged and never appropriated treated.
Regardless, all of this information should at least get you to question the value of surgery for most knee pain complaints. This is not to say that surgery is always a bad option, but you should darn well try something effective first.
This is the end of part 1 of this article. In part 2, I’ll cover what to do INSTEAD of drugs and surgery (or at least what to try first). I’ll also go over the research on certain supplements and vitamins that have been shown to help with arthritis knee pain relief.
Stay tuned!
 Sign up for Bogash Life ‘N Balance and instantly receive a free copy of the eBook:
Sign up for Bogash Life ‘N Balance and instantly receive a free copy of the eBook:
Fantastic article.
Cindy,
Thanks for the feedback!
Dr. Bogash
As I sit here almost 30 days to the date from my meniscus surgery… my pain is “maybe” a little better… Looking forward to part 2 of the article … finally decided to do P.T. and that starts today. I don’t need W.C. telling me down the road that I didn’t do everything possible to correct the problem…